A Culture of Customer Service
Marshall M. Baker, MS, FACMPE
Physician Advisory Services, Inc., Boise, ID
Customer service is a frequently heard buzz word, the “culture” many ad- vocate, and, in the final analysis, the true demonstration of “walking the talk”.
Some will differ on whom they identify as their “customer” – for some anesthesia providers the response is often “the surgeon,” while most acknowl- edge their customer base includes a variety of individuals and organizations – patients, surgeons and proceduralists, hospital and health system administra- tors, surgery center directors, vendors, and members of the payor community. I submit that all of those listed and any others you interact with are “your cus- tomers” – they are whom you serve.
The key is whether these customers view your practice as customer friendly?

What is the level of satisfaction your customers have with your services?
Satisfaction surveying is encouraged and, while approaches vary, the goal is to better understand how you and your group are viewed (and rated).
Surveying techniques include telephone, focus group, written questionnaires, and the disciplined recording of “feedback” as it is received.
Some types of “satisfaction surveying” include:
- Patient Satisfaction (with the experience with their anesthesia provider)
- Surgeon/Proceduralist Satisfaction (with your service, responsiveness)
- Staff Satisfaction (both anesthesia group and delivery site (hospital, ASC, Endoscopy Center, birthing center, etc.) – about their experiences working with you (as clinical support or administrative support staff for you)
- Payors (what’s the “temperature of the water” when you or your staff interact with payors and their staff?)
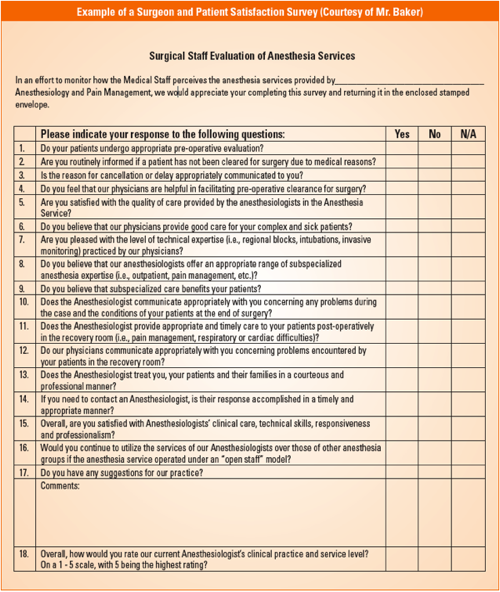
Assessment is one tool that will produce information to either reenforce that a high level of satisfaction exists, or alert you to areas (and individuals) where there are opportunities for improvement. Examples of surgeon and patient satisfaction surveys appear on pages 7 and 8.
In addition to “after the experience” satisfaction surveying, customer service initiatives should be proactive. Here there are a variety of actions or initiatives the group might consider to build a loyal and supportive following. Two that I found produced positive results:
- The anesthesiology group I was associated with instituted a “thank you card” program – our anesthesia providers would leave a card at the patient’s bedside when making post-op/post-procedure rounds. The card read:
THANK YOU for allowing us to be of service to you. We are committed to a healthy community. If you have questions about the care we provided – call: XXX-XXXX If you have questions about payment of our charges – call: YYY-YYYY Anesthesia Consultants, PCThe key here was two-fold, to genuinely thank the patient and to reinforce that we had been involved in their care – patients always remember their surgeon/proceduralist; but seldom recall the name of their anesthesia provider or the group that provided the anesthesia. In fact, many challenge the charges when received and it’s not uncommon to receive a call with the patient stating, “I never saw that doctor”. The card (with the anesthesia provider’s business card enclosed) can minimize those types of calls.
- Another proactive approach we took was the recognition of every surgeon’s birthday – sending a card and a small gift (e.g. – one year it was a mag-lite flashlight, another a small tool kit, with our logo emblazoned on the item).
First, the surgeons were impressed—one remarking, “My mother doesn’t even remember my birthday”.
But the really positive result was when we were battling with insurance companies for payment for post-op pain management and consultation, and the payors threatened to reduce the surgeon’s allowable charge to pay for pain management.
The surgeons rose to our defense (a new behavior in our community where relationships between anesthesiologists and surgeons often disrespect). Because of our positive relationship building activities (only one of which was the birthday gift), they advised the payors that requesting a “pain specialist” for their patient was no different than requesting a consult from any other sub-specialist, and such consultation and service was NOT a part of the surgical or procedural event.
Beyond surveying, cards, or gifts the theme you want to communicate to your customers is the way you and your colleagues treat people.
When there is an inappropriate behavior, how does your practice address it?
Like all communication, it is how the individual interprets your words or actions; and whether such disruptive and inappropriate behavior is viewed as such by you as well as by the customer.
Paramount to such a disruptive or inappropriate behavior is how your group responds. Is such behavior allowed to continue without intervention?
I would suggest a NO tolerance policy for outbursts, “scream-fests”, or deliberate disregard for “driving outside the lines” of established group culture and behavior. The development of a disruptive behavior protocol will be important to assure there is no misunderstanding about what is expected.
When an event occurs, there must be immediate action, and a process to coach the individual toward a change in behavior, with understanding of the consequences if there is no demonstrated change and improvement. To ignore these types of misbehaviors can result in a potential loss of business, damage to the group’s reputation, or worse, litigation.
Customer service should be a hallmark for your practice, and taking the time to craft a customer service program and instill a culture that is readily recognized as “customer friendly” for your organization will be a cornerstone to the long term success of your practice.