Journey to Quality: Quantum Clinical Navigation System
Ruth D. Morton, Ph.D.
Vice President, Anesthesiologists Associated Inc.
Background
More than ten years ago Southeast Anesthesiology Consultants (SAC) Chairman and CEO Richard L. Gilbert (MD, MBA) faced a challenge—making sure surgeons recognized that anesthesiology providers were not the cause of delays and cancellations in the OR. While surgeons could provide only anecdotal cases it was clear that having all the data was essential. This led his group to start a methodical process of incident-based data collection on every case. The process of tracking every patient and measuring the causes of cancellations and delays allowed SAC to prove that the anesthesiologists were rarely the cause of the problem. Not only could the group pinpoint the causes of delays and cancellations but also the system facilitated further opportunities for improvement. This marked the start of the group’s “journey to quality.”
A few years later the Institute of Medicine published To Err is Human, which revealed that as many as 98,000 hospital patients die each year from preventable medical errors (Institute of Medicine, To Err is Human: Building a Safer Health System, 1999). The publication captured the attention of SAC members, and they saw opportunities for improving care provided through their practice. Near that time the group decided to send Dr. Gilbert to an MBA program, where he learned about quality improvement methodologies such as Six Sigma and the Deming Cycle. He worked with his group to apply these quality concepts and tools to their practice. Together they defined metrics, tested them, and refined a data collection tool, resulting in a patient focused and systems oriented approach to quality improvement.
Along with the data collection tool and the software to store and report the data, SAC developed the infrastructure to support their journey to quality. They:
- created a Continuous Quality Improvement (CQI) Committee (at each site and corporate-wide) that reviews results,
- selected a Quality Director who oversees the overall process and facilitates its coordination,
- hired and placed QA nurses at high volume locations who work seamlessly in the hospital environment, function as members of the anesthesia department, monitor the data-input process and collect data on patient satisfaction,
- initiated email alerts that go to practitioners when they’ve exceeded thresholds on quality indicators, or to practitioners, or to the CQI Committee and department chief upon critical events (i.e. stroke or cardiac arrest), and
- developed educational materials, interventions, and mentoring processes that help providers learn better and safer techniques and protocols.
Results
Today SAC, a 75+ member group that practices in North Carolina, South Carolina, and Virginia, is proud of their investment in quality improvement and the results they have achieved throughout their journey. Their CQI software is now called the Quantum Clinical Navigation System™ (Quantum CNS). The patent-pending process includes a 50-indicator checklist that tracks patient satisfaction, OR efficiency, practitioner performance, and clinical outcomes along the Perioperative care continuum. “Ultimately”, says Dr. Gilbert, “doctors and nurses want to deliver outstanding care, and this helps them do it. The Quantum Clinical Navigation System™ provides real time positive and negative feedback loops to individual providers to improve their practice. In addition, the data collected in aggregate across the group is analyzed and along with evidence based medicine, provides the foundation for a systems approach to decreasing medical errors. Our focus has been on demonstrable quality customer satisfaction and efficiency; this has given us the ability to quantify and continually improve. It drives our practice and supports the growth of our business.” He adds: “The real mileage comes from the group taking the information to implement system-wide best practices.”
Tangible
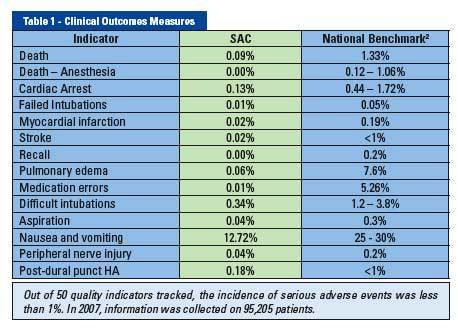
2 National Benchmarks from the IOM Report, MEDLINE, and Evidence-Based Practice of Anesthesiology
By implementing this system, SAC has achieved consistently high results for patient satisfaction (patient satisfaction scored in the high nineties over the last 8 survey years) and consistently exceeded national benchmarks for error reduction and improved outcomes (see Table 1).
In addition to exceeding national benchmarks, SAC’s efforts have tangibly paid off in an 8-10% reduction in its medical malpractice rates in each of the past two years. They have used the lower complication rates reported by Quantum to demonstrate cost savings to managed care companies supporting better reimbursement rates for the Group. The value the group has shown helped them win business with hospitals that are focused on CMS initiatives and on attracting surgeons. Dr. Gilbert notes that approximately 65% of hospital revenue and profit is from the OR. Although anesthesia is small in terms of cost to the hospital, it is a lynchpin to its overall success. And surgeons want skilled anesthesiologists in the OR. As reported in the Clinical Advisory Board Essay, 57% of responding surgeons scored “availability of skilled anesthesiologists” as extremely important, among the top three attributes of 47 possible (Clinical Advisory Board Essay: The State of Hospital-Physician Relations, 2003, p.54). SAC has the data to prove their skills.
Intangible
While the group’s journey to quality has resulted in economic gain for all stakeholders, the journey for individual practitioners has intangible rewards, as well. Overall, providers are pleased with getting rapid and detailed results (data are collected real-time, not by claims data or retrospectively) so they can take timely and effective action. For example, a new group member exceeded a threshold shortly after he started practicing with the group. His high incidence of wet taps was captured by the Quantum Clinical Navigation System™. The provider was then mentored by a skilled peer who taught him better technique. The physician recognized the technique issues, and was glad to get help and support that was provided in a positive manner. Improved epidural outcomes were also captured by Quantum and tracked for continual assessment. Quality Director Janet Beck notes that the use of Quantum Clinical Navigation System™ resulted in timely identification of the issue, intervention, and ultimately behavior change. Without a mechanism for early intervention, the physician may have improved his technique over time, but it would have taken longer and affected more patients.
Another example of an intangible reward was at a location having lower scores for labor pain control in OB. A team including the department chief, QA nurse, and the quality director analyzed the data and found differences between anesthesia providers. This led to the physicians at the location (those with higher and lower scores) talking among themselves. Their collaboration and teaming led to lower scoring doctors recognizing the differences in how they were treating labor pain. The care team also found out that nursing staff needed to better educate the patients on use of the IV pain medication control. Subsequently, the patient satisfaction scores went up significantly in only three months for that location.
Hospital Partnership
In an era when hospitals are under the pinch to achieve quality measures, they ask for quality anesthesia practitioners who can help them achieve certain CMS-SCIP, JCAHO, and IOM initiatives. Southeast Anesthesiology’s use of their Clinical Navigation System™ has given them a head start in providing necessary data for hospitals where they practice. With the trend toward transparency of outcomes, data from Quantum has helped SAC partner with hospitals to deliver outstanding care. And, Quantum CNS has been a vehicle for providing evidence that stipends paid to the group are worth it for the hospital.
Data from use of Quantum CNS has helped physicians and hospitals implement best practices such as:
- standing orders for pain control
- process improvements to minimize central line infection
- early eye protection protocol to prevent corneal abrasion
- implementation of obstructive sleep apnea protocol
- improved labeling to reduce medication errors
- clinical initiatives to reduce anesthesia recall
- protocols to improve control of labor pain
- protocols to lower the incidence of post op nausea and vomiting
Educational Approach
Quality Director Beck believes that Southeast’s leadership in educating physicians is one of the keys to the success of the quality program at SAC. She emphasizes:
- the quality process and the cycle of quality improvement,
- peer review and its importance, and
- Pay for Performance — why it is coming and how to prepare.
Ms. Beck indicates that data generated through use of Quantum CNS is used by SAC in an educational way. Improvement is achieved through learning—the use of mentors, educational materials, and processes. For example, they have created educational modules for sleep apnea and preoperative beta blocker administration. The data is not used for punitive purposes. If a threshold is exceeded and the system sends an automatically generated alert that a practitioner is not following a protocol, the individual is given a set of educational slides to review. Or, in the case of an individual with low patient satisfaction scores related to communication skills, the physician may attend a series of educational communication sessions, and scores are monitored for a time following the educational sessions. Ms. Beck relays that it is “very gratifying for individuals to see improvement on their measures.”
Over the years of their journey to quality, there have been challenges. The initial challenge was inertia – the usual phenomena of resistance to change, even when the change is considered good. Then practitioners doubted the completeness of the data until they understood that it was not just sampling. A third challenge was getting providers to change behavior based on the data. And, a final challenge was getting members to believe the improved results. A sound scientific approach combined with a positive, non-punitive educational environment successfully guided the practice through these challenges. Continuing the education of nurses, CRNAs, and anesthesiologists, with Quantum CNS providing data to drive the practice, has successfully led the group members to see themselves as a “high performance practice.”
Quantum CNS Available to Anesthesia Groups and Hospitals
In 2008, SAC entered into an agreement with Anesthesia Business Consultants to make Quantum CNS available to ABC’s existing billing clients and to promote it to anesthesia groups and hospitals nationwide.
Small to large anesthesia practices and hospitals can avail themselves of the benefits of this CQI software without investing the time or money to develop it. It can be purchased as a package with their ABC billing services, or as a stand-alone service through licensing and per case fees. Dr. Gilbert states that critical mass is not necessary to implement Quantum CNS and infrastructure needs are limited. From a user perspective, it does not take much time to learn or to enter the data. However, what is necessary is the commitment from group or hospital leaders to embrace the journey to quality.
Quantum CNS is currently in use at Carolinas Healthcare System in North Carolina, Sentara Hospital System in Virginia, and Community Health Systems in South Carolina. The system, designed by clinicians for clinicians, has been field tested at these sites, which range from tertiary-care medical centers to rural hospitals.
Why Might Oher Hospitals and Anesthesia Groups Want to Use Quantum CNS?
Among other reasons, Gilbert writes that “Every health care provider in America wants to assert that he or she provides high-quality services. The proof is in the results. Also, it is clear that pay for performance is here to stay. Embracing a rigorous CQI program that integrates a systems approach to clinical care, quantifies key metrics, and communicates them effectively can position medical groups to turn the potential threat of pay for performance into an opportunity.”(MGMA Connexion, September 2006, page 24)
Return on Investment
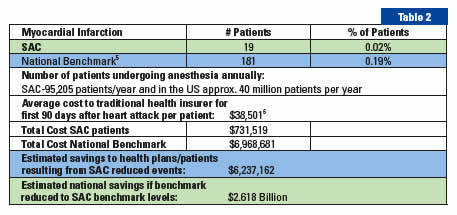
The return on investment for a program such as this benefits all parties including patients, providers, hospitals, and managed care companies. Savings on just one indicator alone—Myocardial Infarction—of the 50 indicators in Quantum CNS are calculated in Table 2.
5 Chung, Dorothy and Stevens, Robert, Evidence-based Practice of Anesthesiology, page 379.
6 NBER Working Paper No. 6514, nber.org/digest/Oct 98, National Bureau of Economic Research
High-Performance Healthcare
The use of Quantum’s Clinical Navigation System™ creates an environment where medical professionals and institutions can achieve true high-performance healthcare – the reason behind the journey to quality. On the journey, you can reduce medical errors, change clinician behaviors, enhance quality of care, run more efficient OR operations, maximize managed care reimbursement, and even lower malpractice insurance premiums. And, Quantum CNS paves the path toward Pay for Performance.

For more information
To get more information and to explore how you can start or continue your journey to quality using Quantum CNS, contact Anesthesia Business Consultants at 517.787.6440, Extension 4113.