What Anesthesiologists And Pain Management Physicians Need To Know About The RAC Program
Abby Pendleton, Esq., and Jessica L. Gustafson, Esq.
The Health Law Partners, P.C., Southfield, MI
Anesthesiologists and pain management physicians, like other Medicare providers, should be prepared for increased Medicare auditing activity. The Centers for Medicare and Medicaid Services (CMS) Recovery Audit Contractor (RAC) program has been made permanent and is expanding nationwide, and the RACs will begin auditing in the very near future. Medicare providers should be aware that RAC claim denials and overpayment demands, like other Medicare denials, can be appealed through the standard Medicare appeals process.
1. RECOVERY AUDIT CONTRACTORS
Section 306 of the Medicare Prescription Drug, Improvement and Modernization Act of 2003 (MMA) directed the Department of Health and Human Services (HHS) to conduct a three-year demonstration program using RACs. The demonstration began in 2005 in the three states with the highest Medicare expenditures: California, Florida and New York. In 2007, the demonstration expanded to include Massachusetts, South Carolina and Arizona. The purpose of the RAC demonstration program was to determine whether the use of RACs would be a cost-effective way to identify and correct improper payments in the Medicare program.
The RAC demonstration program proved highly “cost effective” to CMS. Over the three-year demonstration, the RACs identified more than $1.03 billion in improper payments. The vast majority of this amount, $992.7 million, constituted alleged overpayments. According to CMS, factoring in the underpayments returned to providers and suppliers ($37.8 million), the claims overturned on appeal ($46 million), the amounts improperly recouped and returned to providers upon re-review ($14 million) and the operating costs of the demonstration program ($201.3 million), the RAC program was successful in returning $693.6 million to the Medicare Trust Funds. CMS estimates that the RAC demonstration program cost approximately 20 cents for each dollar returned to the Medicare Trust Funds.1
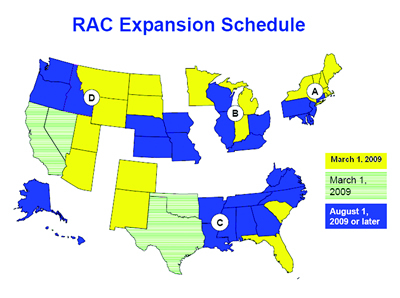
Section 302 of the Tax Relief and Health Care Act of 2006 made the RAC program permanent, and required its expansion nationwide by no later than 2010. CMS is actively moving forward with this expansion. According to its most-recently published “Expansion Schedule,” CMS planned to expand to 23 states by March 1, 2009, and the remaining states by August 1, 2009 or later.2
On October 6, 2008, CMS announced the names of the RAC vendors for the permanent program, and identified the initial states for which each will be responsible:
- Diversified Collection Services, Inc., of Livermore, California is the RAC for Region A, including Maine, New Hampshire, Vermont, Massachusetts, Rhode Island and New York;
- CGI Technologies and Solutions, Inc. of Fairfax, Virginia is the RAC for Region B, including Michigan, Indiana and Minnesota;
- Connolly Consulting Associates, Inc. of Wilton, Connecticut is the RAC for Region C, including South Carolina, Florida, Colorado and New Mexico; and
- HealthDataInsights, Inc. of Las Vegas, Nevada is the RAC for Region D, including Montana, Wyoming, North Dakota, South Dakota, Utah and Arizona.3
More information is available from the CMS RAC website: www.cms.hhs.gov/RAC.
Before the permanent RACs begin auditing, the RACs announced they would hold “Town Hall”-type outreach meetings, at which the RACs and CMS representatives would meet with Medicare providers and suppliers. According to recent conversations this office had with Commander Marie Casey, Deputy Director of the CMS Division of Recovery Audit Operations, Medicare providers and suppliers in the first 23 states can expect automated reviews (electronic review of claims data records that do not involve a review of medical records) to begin at any time. Complex reviews (where medical records are requested) will begin for coding issues in September 2009, and medical necessity reviews will begin in January 2010.
CMS compensates RACs on a contingency fee basis, based upon the principal amount of collection from (or the amount repaid to) a provider. This fee arrangement provides incentive to the RAC to aggressively review and deny claims, including claims that the RAC alleges to be not “medically necessary,” an area containing much subjectivity, and a category of denial often highly disputed by the provider.4 RACs are permitted to attempt to identify improper payments resulting from any of the following:
- Incorrect payments;
- Non-covered services (including services that are not reasonable and necessary);
- Incorrectly coded services; and
- Duplicate services.5
When performing coverage or coding reviews of medical records, nurses (RNs) or therapists are required to make determinations regarding medical necessity, and certified coders are required to make coding determinations. The RACs are not required to involve physicians in the medical record review process. However, the RACs must employ a minimum of one FTE contractor medical director (CMD) (who must be a doctor of medicine or doctor of osteopathy) and arrange for an alternate CMD in the event that the CMD is unavailable for an extended period. The CMD will provide services such as providing guidance to RAC staff regarding interpretation of Medicare policy.
Although the RACs have fairly broad discretion in determining which claims to review, CMS has prohibited the RACs from looking at certain categories of claims. For example:
- The permanent RAC program will begin with a review of claims paid on or after October 1, 2007. This first permissible date for claims review is the same for the RAC reviews in all states, regardless of the actual start date for a RAC in a particular state. However, as time passes, the RACs will be prohibited from reviewing claims more than three years past the date of initial determination (defined as the initial claim paid date).
- RACs are not permitted to review claims at random. However, RACs are authorized to use “data analysis techniques” to identify claims likely to be overpayments, a process called “targeted review.” In the demonstration program, the “targeted review” resulted in certain categories of providers and certain types of claims being subject to more scrutiny than others.6
2. IMPACT OF RAC AUDITS
Over the course of the three-year demonstration, the RACs identified and collected $992.7 million in overpayments and ordered repayment of just $37.8 million in underpayments to Medicare providers and suppliers.7 Thus, approximately 96 percent of the alleged improper payments identified were overpayments, as opposed to underpayments.
3. PREPARING FOR A RAC AUDIT
Medicare providers, including anesthesiologists and pain management physicians, should begin to prepare now for the RACs and increased Medicare auditing activity. Although providers cannot prevent RAC audits from happening, they can prepare for increased claims scrutiny and RAC activity by dedicating resources to:
- Internal monitoring protocols to better identify and monitor areas that may be subject to review (i.e., reviewing compliance guidance documents such as RAC Evaluation Reports, the OIG Work Plan and OIG compliance guidance, and dedicating resources to monitoring compliance risk areas);
- Responding to record requests within the required timeframes;
- Implementing an effective compliance program in accordance with OIG guidelines, and/or strengthening procedures currently in place.
Pursuant to the “Update to the Evaluation of the 3-Year Demonstration,” published in January 2009, “Future improper payments can be avoided by analyzing the RACs’ service-specific findings.”8 Looking to the results of the RAC demonstration program is not particularly illustrative or educational for anesthesia providers and pain management physicians, however. This is because:
- The vast majority of RAC claim denials in the demonstration program involved Part A hospital claims. Eighty-five percent of the claims reviewed in the RAC demonstration program were inpatient hospital claims (e.g., short stays and DRG coding issues);
- Six percent of the claims were inpatient rehabilitation facility claims; 4.25 percent of the claims were outpatient hospital claims;
- Two and one-half percent of the claims were physician claims;
- One and three-quarters percent of the claims were skilled nursing facility claims; and
- One percent of the claims involved DME, ambulance, lab and other services.
Although the historical information regarding RAC denials is not particularly illustrative to anesthesiologists and pain management physicians, there is other program guidance identifying areas of increased claims scrutiny. For example, each year the OIG publishes a Work Plan setting forth various projects to be addressed during the upcoming fiscal year, to which the RACs may look to identify potential areas for their audit activities. In 2008, the OIG Work Plan identified interventional pain management procedures as procedures likely to undergo claims scrutiny for medical necessity. The OIG noted that interventional pain management is a growing specialty, and Medicare paid nearly $2 billion for interventional pain management procedures in 2005.
In addition to the OIG Work Plan, in September 2008, the OIG issued a report on “Medicare Payments for Facet Joint Injection Services.” The report stated that the OIG had found that 63 percent of facet joint injection services allowed by Medicare in 2006 did not meet Medicare program requirements, resulting in $96 million in improper payments.
Although the information from the RAC demonstration program does not provide specific guidance for the anesthesia and pain management industries in terms of strategic planning for the permanent program, taking into account other available guidance, anesthesia and pain groups are well advised to strengthen their compliance programs to ensure that certain anesthesia and pain management focus areas are enhanced. For example, groups should ensure that:
- Each provider is only capturing allowable anesthesia time and that appropriate documentation exists to support the recorded start and end times;
- Compliance with the medical direction requirements is satisfied, including enhancing documentation practices to demonstrate such compliance;
- Documentation practices are improved with regard to separately payable services such as invasive monitoring lines and post-operative pain services;
- Documentation practices are improved with regard to medical necessity documentation in connection with the performance of monitored anesthesia care cases;
- Documentation practices are improved with regard to medical necessity documentation in connection with the provision of chronic pain management procedures; and
- Documentation practices are improved with regard to medical necessity documentation relative to the provision of evaluation and management services.
4. WHAT TO EXPECT IF YOU ARE AUDITED BY A RAC
RACs engage in two types of claim reviews to identify improper payments: “automated review” and “complex review:”
An “automated review” is a review of claims data without a review of the records supporting the claim. Generally speaking, RACs may conduct automated reviews only in situations where there exists both (a) a certainty that the service is not covered or is incorrectly coded, and (b) a written Medicare policy, article, or coding guideline applicable to the claim. RACs also may use automated review, even if there is no specific Medicare policy, article or coding guideline on point, in some “clinically unbelievable” situations9 or when identifying duplicate claims and/or pricing mistakes.10 According to Commander Marie Casey, Deputy Director of the Division of Recovery Audit Operations at CMS, automated reviews of providers in the first 23 states can be expected to begin at any time.
On the other hand, a “complex review” consists of a review of medical or other records, and is used in situations where there is a high probability (but not a certainty) that a claim includes an overpayment.11 In summary, the RAC “complex review” process is as follows:
- RACs are authorized to: (a) visit the provider’s location to view and/or copy medical records or (b) request that the provider mail, fax, or otherwise securely transmit the records to obtain medical records necessary to conduct claim reviews. To “securely transmit” medical records means to send those records “in accordance with the CMS business systems security manual – e.g., mailed CD, MDCN line, through a clearinghouse).12
During the RAC demonstration program, some providers were overwhelmed by the volume of records requests received from the RACs. In the permanent program, CMS imposed limits on the number of records RACs may request per 45-day period.13 For physicians, such as anesthesiologists and pain management physicians, this record request limit is as follows:
- Solo Practitioner: 10 medical records per 45 days
- Partnership of 2-5 individuals: 20 medical records per 45 days
- Group of 6-15 individuals: 30 medical records per 45 days
- Large Group (16+ individuals): 50 medical records per 45 days.14
It is essential that providers timely respond to RACs’ requests for medical records. If a RAC does not receive requested medical records within 45 days, it is authorized to render an overpayment determination with respect to the underlying claim.15 If the provider appeals this type of denial, “the appeals department may, at CMS direction, send the claim to the RAC for reopening under certain conditions…”16 However, the Carrier or Intermediary is not required to send the claim to the RAC for reopening. Thus, providers failing to timely respond to RACs’ medical records requests could lose appeal rights with respect to these claims.
- Once requested medical records are received, the RAC will conduct its review of the claim. In conducting reviews, RACs are required to comply with National Coverage Decisions (“NCDs”), Coverage Provisions in Interpretive Manuals, national coverage and coding articles, Local Coverage Decisions (“LCDs”), and local coverage and coding articles in their respective jurisdictions.17 The RACs also are authorized to develop internal guidelines to assist their reviewers to conduct claims reviews consistently with NCDs and LCDs.18
- Generally speaking, a RAC must complete complex reviews within 60 days from receipt of the requested medical records.19 Following its review, the RAC will issue a letter to the provider setting forth the findings for each claim and notifying the provider of its appeal rights. Alleged overpayments identified by RACs may be appealed through the uniform Medicare appeals process.
According to Commander Casey, complex reviews regarding certain coding issues are planned to begin in September 2009. Complex reviews regarding issues of medical necessity will begin sometime after January 1, 2010.
5. HOW TO APPEAL CLAIMS DENIED BY A RAC
RAC denials are subject to the standard Medicare appeals process set forth in 42 C.F.R. Part 405, subpart I.
A. Stage 1: Redetermination
The first level in the appeals process is redetermination. Providers must submit redetermination requests in writing within 120 calendar days of receiving notice of initial determination. There is no amount in controversy requirement.
B. Stage 2: Reconsideration
Providers dissatisfied with a carrier’s redetermination decision may file a request for reconsideration to be conducted by a Qualified Independent Contractor (QIC). A QIC is a Medicare contractor tasked to complete the second level of appeal (reconsideration level of appeal). This second level of appeal must be filed within 180 calendar days of receiving notice of the redetermination decision. There is no amount in controversy requirement.

Of particular note, providers must submit a full and early presentation of evidence in the reconsideration stage. When filing a reconsideration request, a provider must present evidence and allegations related to the dispute and explain the reasons for the disagreement with the initial determination and redetermination. Absent good cause, failure of a provider to submit evidence prior to the issuance of the notice of reconsideration precludes subsequent consideration of the evidence. Accordingly, providers may be prohibited from introducing evidence in later stages of the appeals process if such evidence was not presented at the reconsideration stage.
C. Stage 3: Administrative Law Judge Hearing
The third level of appeal is the Administrative Law Judge (ALJ) hearing. A provider dissatisfied with a reconsideration decision or who has exercised the escalation provision at the reconsideration stage may request an ALJ hearing. The request must be filed within 60 days following receipt of the QIC’s decision and must meet the amount in controversy requirement. ALJ hearings can be conducted by video-teleconference (VTC), in-person, or by telephone. The regulations require the hearing to be conducted by VTC if the technology is available; however, if VTC is unavailable or in other extraordinary circumstances the ALJ may hold an in-person hearing. Additionally, the ALJ may offer a telephone hearing.
D. Stage 4: Medicare Appeals Council Review
The fourth level of appeal is the Medicare Appeals Council (MAC) Review. The MAC is within the Departmental Appeals Board of the U.S. Department of Health and Human Services. A MAC Review request must be filed within 60 days following receipt of the ALJ’s decision. Among other requirements, a request for MAC Review must identify and explain the parts of the ALJ action with which the party disagrees. Unless the request is from an un-represented beneficiary, the MAC will limit its review to the issues raised in the written request for review.
E. Stage 5: Federal District Court
The final step in the appeals process is judicial review in federal district court. A request for review in district court must be filed within 60 days of receipt of the MAC’s decision.
6. STRATEGIES FOR APPEALING CLAIM DENIALS
Once a provider receives a claim denial made by a RAC, it is important that the provider aggressively pursue appealing the denial through the Medicare appeals process. Experienced healthcare legal counsel can assist providers with appeals to ensure all available substantive challenges and legal theories are utilized. Experienced counsel will submit an appeal brief/position statement that advocates the provider’s position.
7. CONCLUSION
Medicare providers, including anesthesiologists and pain management physicians, should be ready for increased Medicare auditing activity as the RAC program expands nationwide. Providers should make efforts now to evaluate their compliance with Medicare policy. Should a provider be subject to a RAC or other Medicare audit, effective strategies are available that can be successfully employed in the appeals process to challenge claim denials.
Abby Pendleton and Jessica L. Gustafson are partners with the health care law firm of The Health Law Partners, P.C. The firm represents hospitals, physicians, and other health care providers and suppliers with respect to their health care legal needs. Pendleton and Gustafson specialize in a number of areas, including but not limited to: Recovery Audit Contractor (RAC), Medicare, Medicaid and other payor audit appeals, healthcare regulatory matters, compliance matters, reimbursement and contracting matters, transactional and corporate matters, and licensing, staff privilege and payor de-participation matters. They can be reached at apendleton@thehlp.com and jgustafson@thehlp.com.
1 The Medicare Recovery Audit Contractor (RAC) Program: An Evaluation of the 3-Year Demonstration,” at p. 15, June 2008, available at www.cms.hhs.gov.
2 RAC Expansion Schedule, available at www.cms.hhs.gov.
3 Id. Note that the RAC Expansion Schedule indicates the four RAC regions, labeled A, B, C and D.
4 In a significant change from the demonstration program, under the permanent RAC program, if a provider files an appeal disputing the overpayment determination, and provider wins this appeal at any level, the RAC is not entitled to keep its contingency fee, and must repay CMS the amount it received for the recovery. RAC Statement of Work, available at www.cms.hhs.gov.
5 RAC Statement of Work, available at http://www.cms.hhs.gov/RAC/10_ExpansionStrategy.asp#TopOfPage.
6 Id.
7 “The Medicare Recovery Audit Contractor (RAC) Program: An Evaluation of the 3-Year Demonstration,” at p. 15, June 2008, available at www.cms.hhs.gov.
8 tp://www.cms.hhs.gov/RAC/Downloads/AppealUpdatethrough83108ofRACEvalReport.pdf.
9 A “clinically unbelievable” situation is one where “certainty of noncoverage or incorrectly coding exists but no Medicare policy, Medicare articles or Medicare-sanctioned coding guidelines exist.” In these cases, the RAC may ask CMS to approve automated review. However, unless CMS specifically approves an issue for automated review, the RAC must use complex review to make such determinations. See “Statement of Work for the Recovery Audit Contractor Program” at p. 18, available at www.fbo.gov.
10 Id. at pp. 17-18.
11 Id.
12 Id. at p. 11.
13 Id.
14 See “RAC Medical Record Request Limits,” available at www.cms.hhs.gov
15 See “Statement of Work for the Recovery Audit Contractor Program” at p. 13, available at www.fbo.gov.
16 Id. at p. 20 (emphasis in original).
17 Id. at p. 16.
18 Id. at p. 17.
19 Id. at p. 19.
20 Id. at p. 22.