Anesthesia Industry eAlerts
Sent to subscribers every Monday morning, our eAlerts deliver timely updates on regulatory, legislative and practice management developments of interest to anesthesia professionals.
Complete the simple form below to subscribe.
2010 PQRI Requirements and Anesthesiologists' Choices
January 11, 2010
Do you have any questions about the Physician Quality Reporting Initiative now that we are into 2010? Judging by our e-mails, telephone calls, and client meetings, many anesthesia groups still have basic questions, and the most sophisticated PQRI participants are identifying new gaps in the official PQRI information released by CMS.
Much of the uncertainty centers on the number of PQRI measures that an anesthesiologist must report. As you know, there are now three measures for anesthesiology:
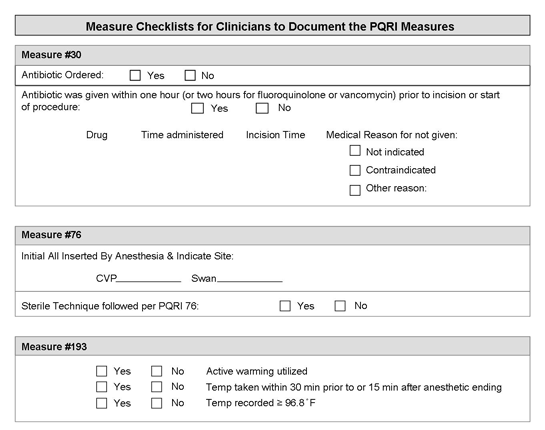
- #30, Perioperative Care: Timely Administration of Prophylactic Parenteral Antibiotics
- #76, Prevention of Catheter-Related Bloodstream Infections (CRBSI): Central Venous Catheter (CVC) Insertion Protocol
- #193, Perioperative Temperature Management
As you have probably also heard, physicians must report a minimum of three PQRI measures if at least three measures are applicable to their practices. If only one or two measures apply, then reporting on just those measures (in at least 80 percent of eligible cases) will qualify for the PQRI bonus. That bonus is once again 2 percent of all the physician’s charges “allowed” by Medicare.
Anesthesiologists do not have to report all three measures, #30, #76 and #193 in order to earn the bonus (although they may choose to do so). It will be sufficient to report:
- Measure #30 and Measure #76, or
- Measure #193 and Measure #76, or
- Measure # 76 alone.
Last year anesthesiologists qualified for the bonus by submitting “quality data codes” (QDCs) for just one measure (#30) on a minimum of 80 percent of their eligible cases. This year they will also have to report Measure #76 successfully. They are not required to report Measure #193 (temperature management) along with #30 (antibiotic prophylaxis), but if they report either or both of those two measures, they will need to report #76 as well.
The explanation for requiring the above code pairs to be reported together can be found in CMS’ Measure Applicability Validation (MAV) process. The MAV process entails a review of all of the Medicare claims submitted by a sample of the physicians who report fewer than three PQRI measures to see if other measures were applicable to those physicians’ practices. Whether a measure applies to an individual physician depends on a 2-part test: (1) a “clinical relation test” to identify other services that the physician might be expected to provide based on the one(s) he has reported, and (2) a minimum threshold number of eligible cases. All that we need to note here about the threshold number of cases is that if the anesthesiologist, for example, performs fewer than 15 central line insertions in 2010, he or she will not need to report Measure #76.
It also bears repeating that if the physician has successfully reported three (or more) PQRI measures, there is no need for a MAV review. If he or she has reported only one or two measures, however, CMS will look at the “measure clusters“ in the MAV system to see whether the clinical relation test is satisfied. “This test is based on: (1) an extension of the statutory presumption that if a professional submits data for a measure, then that measure applies to her/his practice and (2) the concept that if one measure in a cluster of measures related to a particular clinical topic or professional service is applicable to a professional’s practice, then other closely-related measures (measures in that same cluster) may also be applicable.” ( 2009 MAV white paper.)
The 2010 MAV paper lists two measure clusters for anesthesia care:
Measure #30 and Measure #76 – The Simplest Option
Anesthesiologists should be reporting Measures #30 and #76 or #193 and #76 to earn their 2010 PQRI bonuses, as we have now seen. Many anesthesiologists began reporting #30 and #76 in 2009, when these two measures were not paired in any MAV cluster. The simplest option for these physicians will be to continue exactly what they have been doing.
(We would not encourage you to report only #76 and to stop submitting your PQRI-quality data codes on the antibiotic prophylaxis measure. That might be seen as gaming the system and while CMS doesn’t yet have means to deny the PQRI bonus to physicians reporting minimally, it has advised physicians to “Select the reporting option (i.e., reporting individual measures or measures groups) best suited for the practice. [Practitioners] should not choose individual measures that do not or infrequently apply to services provided to Medicare patients by the [practitioner]/practice.”)
Another way to game the system is to default to PQRI modifier 8P, or to add 8P to a high proportion of the PQRI measures reported. Modifier 8P means “action not performed, reason not otherwise specified,” and CMS has stated:
The 8P reporting modifier facilitates reporting an eligible case on a given measure when the clinical action does not apply to a specific encounter. EPs [Eligible Professionals] can use the 8P modifier to receive credit for satisfactory reporting but will not receive credit for performance. EPs should use the 8P reporting modifier judiciously for applicable measures they have selected to report. The 8P modifier may not be used indiscriminately in an attempt to meet satisfactory reporting criteria without regard toward meeting the practice’s quality improvement goals.
As with choosing to report on infrequently-performed procedures, relying on 8P so as not to have to ensure that the prophylactic antibiotic is administered within one hour before incision or appropriately documented (QDC 4049F-8P), for instance, is a temptation of which CMS is aware. Until there is a statutory change, however, CMS cannot prevent use of the 8P modifier, indiscriminate or legitimate.
What about Measure #193, Perioperative Temperature Management?
Whether to develop the protocols and documentation procedures in order to report a third measure depends on your attitude toward the PQRI. Some practices see the PQRI as little more than a source of 2 percent additional Medicare income. These practices will want to minimize the disruption of a new learning curve for their clinicians. Why add to the paperwork load without a new financial incentive?
Other practices may want to report Measure #193, or may in fact be using active warming intraoperatively, but they may nevertheless choose not to add the #193 QDCs to their claim forms because of the documentation burden. If the anesthesiologist wishes to report that he did not use warming techniques because they were medically contraindicated, he must ensure that the medical record shows one of the following reasons:
- intentional hypothermia, or
- active warming not indicated due to anesthetic technique: peripheral nerve block without general anesthesia, or
- monitored anesthesia care
Beyond avoiding the hassle factor of still more documentation, many anesthesiologists and other physicians have experienced the PQRI as opaque and arbitrary. It seems easy to make an innocent documentation mistake and the consequences might be forfeiting their entire PQRI bonus. Why add more documentation hurdles that could cost the practice thousands of dollars without offering any opportunity to increase the bottom line? Why, some groups ask, would they volunteer to give the government any more information?
There are quite a few anesthesiologists who are ready to give the government information on more than the minimum number of PQRI measures – those who believe that reporting meaningful performance metrics and comparing individual practices against benchmark data will drive the quality of medical care higher, and who also accept the PQRI as necessary training wheels. Jerry Stonemetz, MD of the Department of Anesthesiology at Johns Hopkins University and National Medical Director, Anesthesia Services at Hospital Corporation of America stated this view best in a message posted to the MGMA-AAA discussion board of January 8th:
I represent several anesthesia groups who work at HCA hospitals, and we are going to report on all three [PQRI measures]. It doesn't hurt to receive the 2% bonus, but the real reason is that this is just the beginning of quality reporting for reimbursement. It will absolutely become the standard for compensation going forward. I think it is like that MasterCard commercial:
- completing the reporting will result in a 2% bonus which will equal $X
- implementing reporting will cost $Y
- demonstrating that your group is in the 90th percentile is priceless!
Hospitals are striving to understand whether their anesthesia groups are providing a quality product. This is one way to illustrate this definition. (Quoted with permission of the author.)
The American Society of Anesthesiologists has made a major commitment to this vision of the future in the form of the Anesthesia Quality Institute (AQI). The AQI is currently laying the foundation for a national anesthesiology clinical registry to which, we predict, the majority of ASA members will be submitting performance data within a few years. The AQI database is going to become invaluable in helping anesthesiologists satisfy Joint Commission, hospital credentialing, Maintenance of Certification and pay-for-performance requirements in addition to the pay-for-reporting requirements of the PQRI. The PQRI measures that you are reporting today will appear in the National Anesthesia Clinical Outcomes Registry (NACOR).
In the shorter term, we encourage all Medical Group Management Association (MGMA) members to help influence the PQRI by participating in the MGMA’s online survey. The aim of the survey is to “obtain information and feedback about MGMA members' experiences with the PQRI program. This information will assist MGMA in advocating for positive changes to PQRI and similar programs that might be created by Congress and administered by CMS.” Completing the survey should only take about 15 minutes, and you have until January 29.
Also in the near term, we invite all readers who are interested in quality improvement/ benchmarking tools to take a close look at the Quantum Clinical Navigation System. The Quantum system was developed by anesthesiologists for anesthesiologists and contains a 50-indicator checklist tracking patient satisfaction, OR efficiency, practitioner performance and clinical outcomes along the perioperative care continuum. It provides real (and real-time) information on anesthesia quality, going far beyond the PQRI; its indicators do include the three PQRI measures. Its purpose is to give a practice the data to drive and demonstrate its own quality improvement accomplishments. Quantum is a tool that has been tested across hundreds of thousands of cases in mulitple hospitals. To arrange a demonstration, contact info@anesthesiallc.com.
With best wishes,
Tony Mira
President and CEO
Click here to download a PDF of this eAlert