Improving the Documentation of Anesthesia Procedures
Darlene Helmer, CMA, CPC, ACS-AN, CMPE, MBA
Vice President of Provider Education and Training, ABC
Reimbursement pressures for anesthesia practices are continuing to escalate due to fluctuations in our healthcare environment. Safeguarding collections is critical and it has become more important than ever to collect every dollar without leaving anything on the table. Good clinical documentation supports accurate coding and the impending ICD-10 implementation increases that significance. For anesthesia providers to facilitate the reduction of coding errors, it is imperative that they have a sound understanding regarding the relationship between good clinical anesthesia documentation and accurate coding. Incomplete documentation requires a return visit to the provider or a review of the operative report which in turn delays the processing and payment of a claim. Delays in claims processing decreases revenue.
Procedure Undercoding
Lack of detail by the anesthesia provider concerning the procedure description is one of the top reasons for undercoding. Detail is vital for accurate coding and optimal reimbursement. Opening the lines of communication between providers and their surgical colleagues is essential. Discussions between the surgeon and anesthesia provider regarding both procedure and diagnosis descriptions for documentation purposes are critical. Working collectively will become evident with the implementation of ICD-10. Documenting this important information not only assists in accurate coding but saves time, creating an efficient process. Querying the providers and searching operative reports is not only time consuming but causes unnecessary delays in claims submission as well as reimbursement. Operative reports are actually the documentation for the surgeon, not the anesthesia provider. Good clinical documentation should reside in the anesthesia record, not the operative report. In the near future, it is certainly reasonable to expect payers to check that all diagnosis and procedures codes submitted will match for all providers and facilities across the board.
Locatation
The catchy phrase “location, location, location” is touted as vital in real estate, and is, in fact, necessary for good clinical anesthesia documentation. Location becomes even more significant involving ICD-10 coding, as it is required to assist in the selection of the correct diagnosis code. In preparation for next year’s ICD-10 implementation, creating good clinical documentation for both procedures and diagnoses will ease this process.
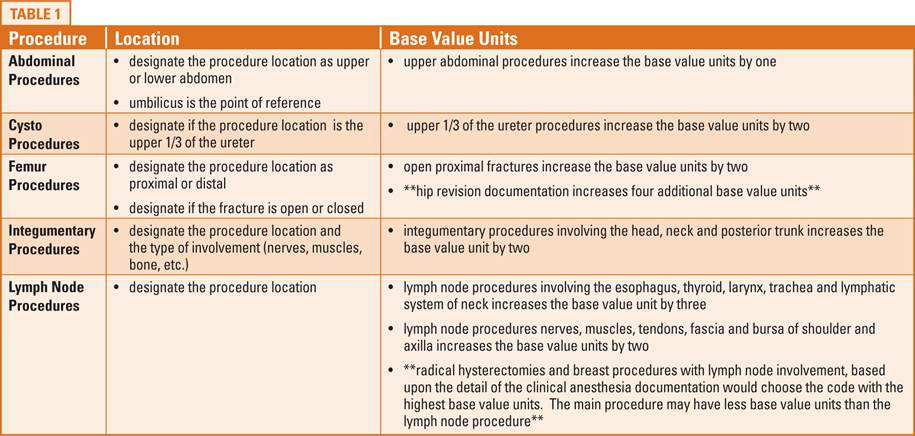
Shown in Table 1 are examples of some common elements of clinical anesthesia documentation that are necessary for accurate coding and optimal reimbursement.
Technique
Good clinical documentation of technique, similarly, is important for accurate anesthesia coding. Shown in Table 2 are examples of the role of technique in anesthesia documentation, coding and, ultimately, optimal reimbursement.
As you can see, there is significant potential to leave many dollars on the table over the course of a year. It is imperative for both the anesthesia providers and coders to embrace continuing education to ensure good clinical documentation and accurate coding. Frequent updated continuing education will both guarantee a reduction of errors and assist in achieving optimal reimbursement. This will safeguard a practice in many ways, especially during an audit where good clinical documentation is readily available to support the coding. Now is a great time to begin practicing these skills so that ICD-10 implementation will be a “piece of cake.”
Darlene F. Helmer, CMA, CPC, ACS-AN, CMPE, MBA serves as Vice President of Provider Education and Training for ABC. She has 30+ years of healthcare financial management and business experience. She works closely with the ABC compliance department and is a member of the ICD-10 training team. She is a long-standing member of MGMA, AHIMA, AAPC and other associations. She is a frequent speaker at local and state conferences. You can reach her at Darlene.Helmer@AnesthesiaLLC.com.